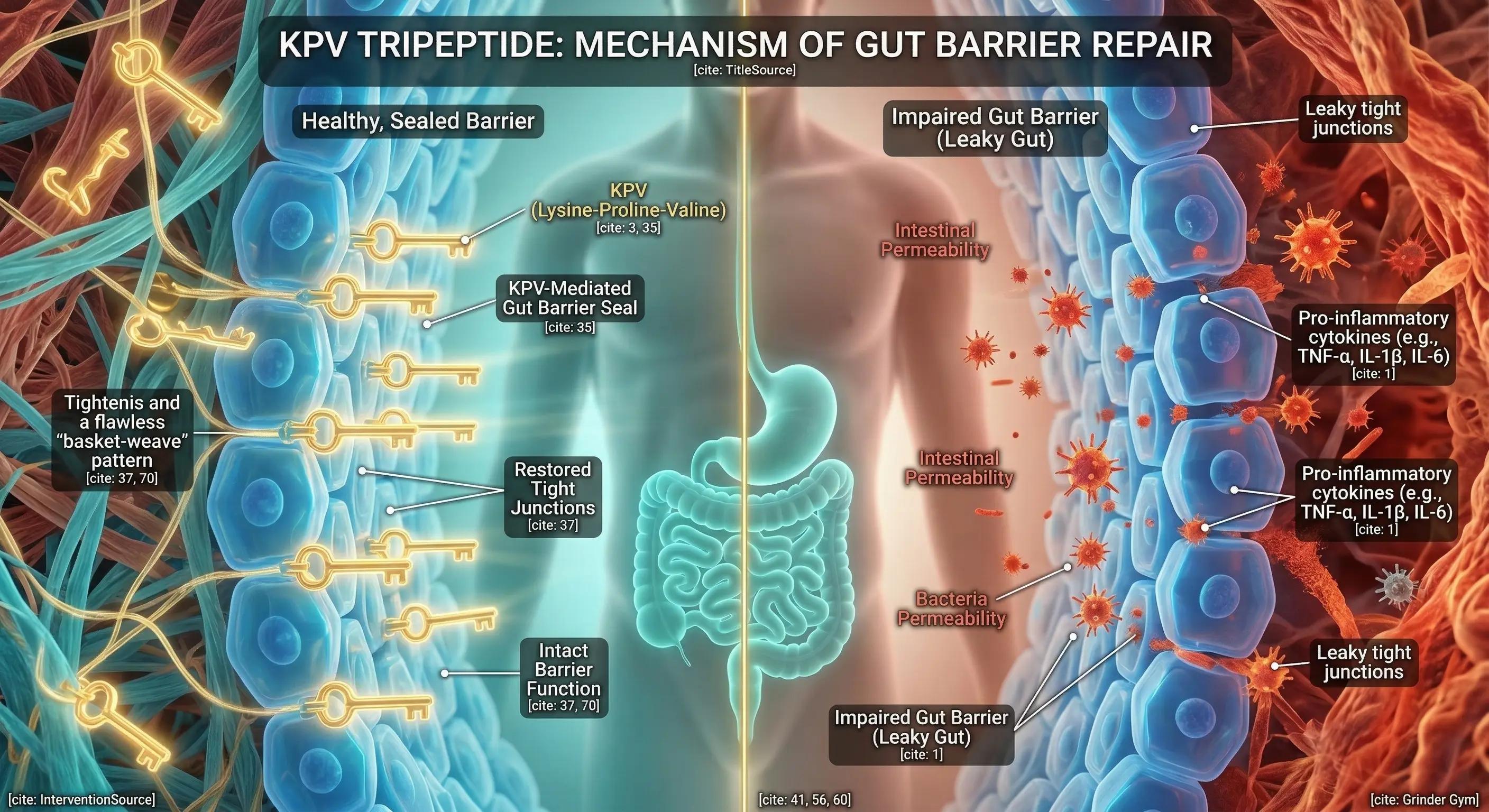
The Role of KPV in Mucosal Inflammation and Gut Microbiota
KPV's Impact on Mucosal Inflammation & Gut Health
Imagine your gut lining acts like a delicate coffee filter, designed to let nutrients pass while blocking harmful toxins. In conditions like Inflammatory Bowel Disease (IBD), this filter tears, creating a state of "leaky gut" where the body’s defenses constantly misfire. This isn't just a stomach ache; it is a physical breakdown of the mucosal barrier, the protective shield that stands between you and disease.
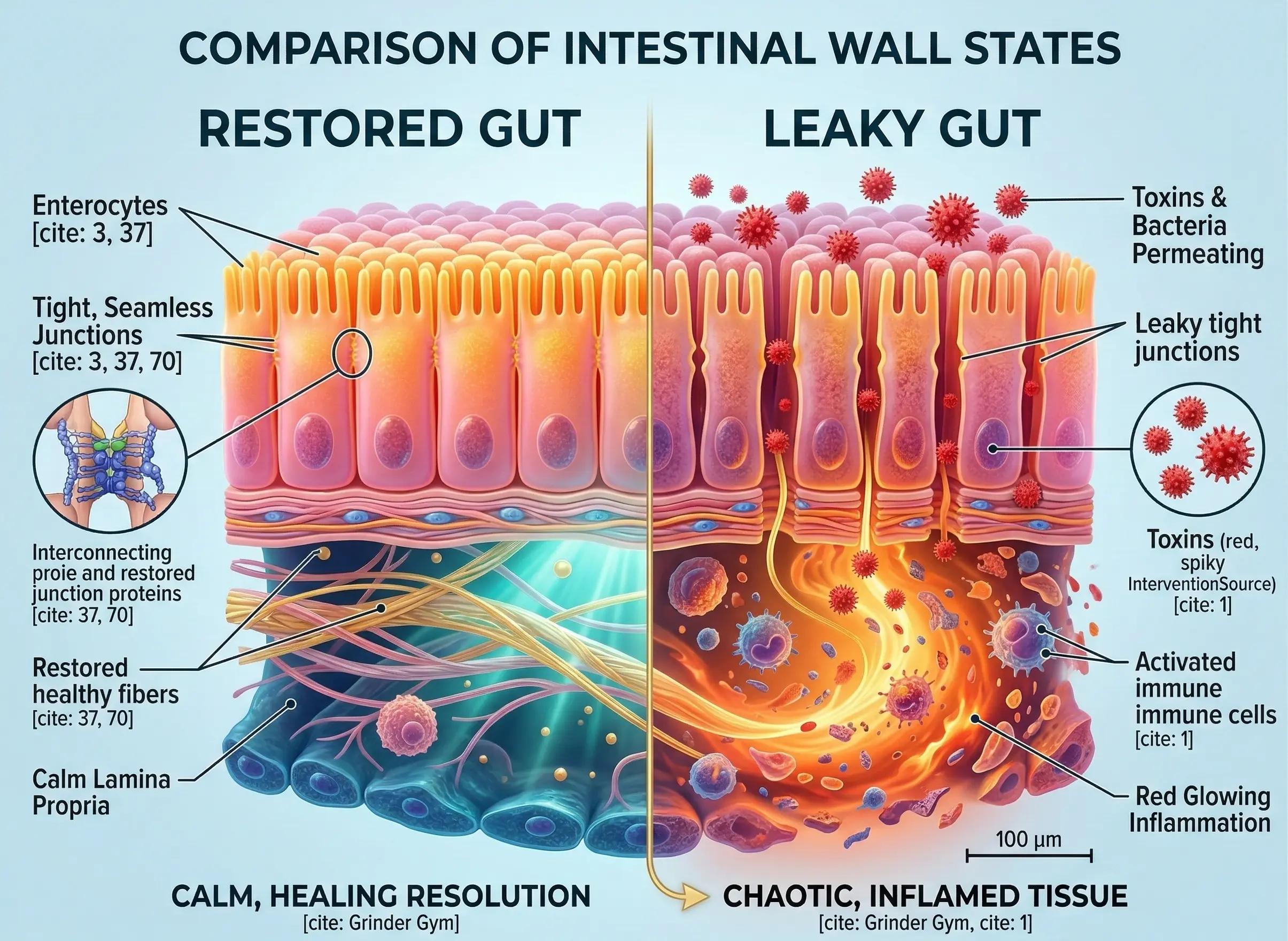
To fix this breach, scientists are investigating a microscopic "master repairman" known as KPV. This naturally occurring tripeptide—essentially a tiny protein fragment—targets mucosal inflammation at its source. Research indicates that instead of simply masking symptoms like traditional steroids might, KPV works to calm the internal fire and actually help rebuild the barrier, offering a promising new frontier for restoring digestive health.
The Mini-Protein Advantage: Why KPV Is Safer and Smarter Than Traditional Treatments
Your body is constantly sending signals to keep things running smoothly. While proteins are the long, complex letters in this communication system, peptides like KPV are the quick, urgent text messages. KPV is technically a "tripeptide," meaning it is a specific sequence of just three amino acids—lysine, proline, and valine. Because it is so small, this molecular messenger can slip easily into cells to deliver its instructions, acting fast to switch off the internal alarms that trigger inflammation.
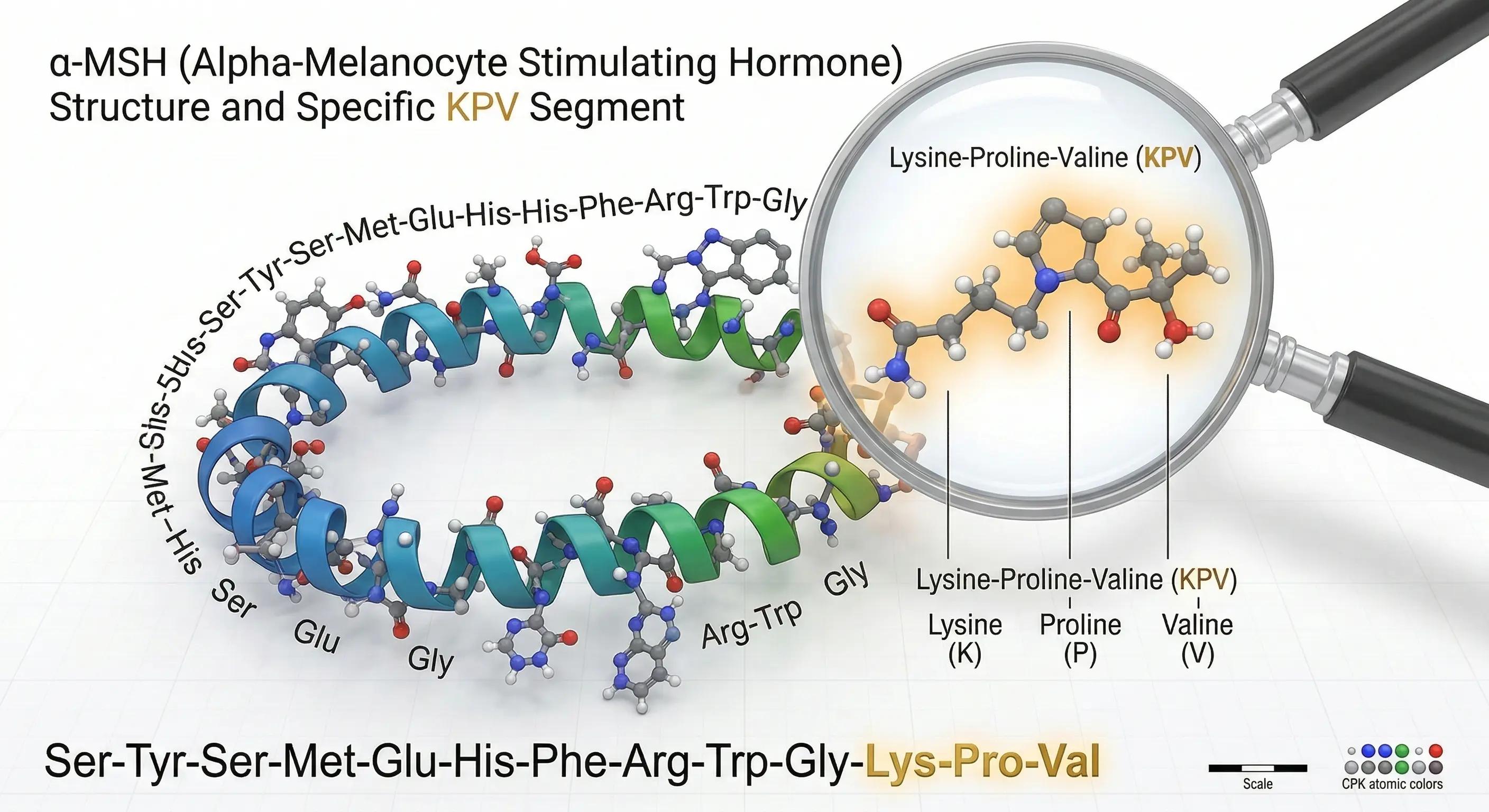
Scientists originally found this powerful sequence hiding inside a larger hormone called alpha-MSH, which is responsible for regulating skin pigment. Although alpha-MSH fights inflammation effectively, using the whole hormone as medicine could unintentionally darken your skin. KPV represents a smarter refinement: researchers isolated only the specific part responsible for calming the immune system. This allows the treatment to deliver the soothing benefits of the parent hormone without the unwanted pigment-changing side effects.
This precision makes the molecule much safer than traditional drugs, which often suppress the entire immune system like a heavy blanket. By functioning as a specific key rather than a sledgehammer, KPV focuses solely on stopping the swelling and redness typical of IBD. Once this inflammatory fire is finally under control, the gut can begin the critical work of repairing its damaged walls.
Fixing the Smart Border: How KPV Actually Heals the Intestinal Wall
Think of the intestinal lining as a frantic emergency room. In conditions like Ulcerative Colitis and Crohn's, the immune system gets stuck in a panic loop, flooding the area with "Red Alert" chemicals known as pro-inflammatory cytokines. These molecular sirens keep the tissue swollen and agitated, preventing recovery. KPV acts as a cellular fire extinguisher; it travels into the cell's "control room" and flips the master switch off, stopping the production of these alarm signals at the source.
Putting out the fire allows the real work of reconstruction to begin. Doctors call this "mucosal healing," and it is the true goal of remission. A healthy gut lining relies on tight junctions—microscopic seals that hold cells together like mortar between bricks. When inflammation eats away at this mortar, the gut becomes "leaky." KPV helps repair these crucial seals, restoring the "smart border" that keeps toxins out while letting nutrients in.
KPV restores this border control through three distinct actions:
- Silencing "Red Alert" chemicals: Halting the cytokine storm that causes ongoing damage.
- Tightening the seals: Repairing the physical tight junctions between cells to close gaps.
- Reducing physical swelling: Allowing the tissue to return to a normal, calm state.
By effectively calming the environment, KPV provides a targeted intestinal mucosal barrier repair method that goes beyond simple pain relief. It transforms the gut from a battleground into a construction site where deep healing can occur. Once this physical foundation is secure, the body is finally ready to address the microscopic residents living within the walls.
A Peacekeeper for Your Gut Garden: How KPV Rebalances Your Internal Bacteria

A healed wall is just the beginning; we must also tend to the trillions of residents living within it. In a healthy digestive tract, diverse bacteria work in harmony to digest food and train immunity, but for IBD patients, this ecosystem often collapses into a chaotic imbalance called dysbiosis. The chronic inflammation described earlier acts like a forest fire, scorching the internal landscape so that helpful bacteria struggle to survive while aggressive, harmful species seize control.
KPV functions here less like a medication and more like a restorative soil conditioner. By dampening the immune system’s overreaction, this peptide creates a safe harbor where beneficial symbiotic bacteria can flourish again. Instead of indiscriminately wiping out microbes as an antibiotic would, KPV helps restore microbiome diversity, allowing the "good guys" to repopulate and naturally crowd out pathogens. This effectively ends the microscopic civil war that often triggers symptoms.
Maintaining this bacterial balance is critical for preventing future flare-ups, as a healthy microbiome acts as a continuing shield against disease. Yet, even the most potent molecule is useless if it is destroyed before arriving at the site of the trouble. The stomach is designed to break down proteins, which presents a major engineering challenge: how to smuggle this delicate peacekeeper past the acidic gauntlet of digestion intact.
Overcoming the Stomach Acid Barrier: How Modern Science Gets KPV Where It’s Needed Most
Creating a pill that works for IBD is surprisingly difficult because the stomach treats most protein-based medicines like food—it breaks them down before they can work. To solve this, researchers have developed microscopic "armored cars" known as nanoparticles. These tiny, engineered carriers encapsulate the KPV peptide, shielding it from the harsh, acidic environment of the upper digestive tract. This advanced technology ensures the medicine remains intact until it reaches the specific area of the intestine where repair is actually needed, transforming a fragile molecule into a robust oral treatment.

This precision approach offers a significant upgrade over traditional treatments, which often flood the entire body with strong medication to reach just one area. By using these smart delivery systems, scientists can achieve three critical goals for safer, easier therapy:
- Acid Protection: Prevents the stomach from digesting the peptide early.
- Targeted Release: Drops the medicine directly on inflamed tissue rather than healthy cells.
- Improved Absorption: Helps the "healing signal" penetrate the mucus layer effectively.
With the delivery puzzle solved, we can now look toward a new era of precision medicine where treatments are both powerful and gentle.
The Future of Gut Health: Why Targeted Mucosal Repair Is the Next Frontier in IBD Care
Understanding IBD requires looking past the symptoms to the cellular "broken shield" within. KPV represents a pivotal shift in this perspective—acting not just as a fire extinguisher, but as a molecular "master repairman" that rebuilds the mucosal barrier and nurtures gut homeostasis. This targeted approach suggests we can move beyond simply suppressing the immune system to actively restoring the delicate balance of your internal ecosystem.
While this is a promising frontier rather than an instant cure, it empowers you to elevate your medical conversations. Instead of focusing solely on pain management, you can now advocate for "mucosal healing" as a true metric of success. As science refines innovative drugs for Crohn's recurrence, watching the evolution of KPV applications in inflammation keeps you connected to the future of IBD treatment—one where healing happens from the inside out.