Accelerating Tissue Remodeling with KPV Tripeptide in Chronic Wound Healing and Scar Prevention
KPV Tripeptide: Enhance Wound Healing & Prevent Scars
We often marvel at the body's ability to heal, but it naturally prioritizes speed over perfection. When you sustain a deep cut or surgical incision, your skin rushes to apply "emergency tape"—a scab—which frequently results in a messy, permanent scar rather than smooth skin. This happens because the biological repair crew often lacks clear direction once the immediate danger has passed.
KPV, a specialized tripeptide—a short chain of just three amino acids—acts like a site manager for your cells. Instead of allowing a disorganized patch job, KPV provides a blueprint for "tissue remodeling," instructing the body to organize collagen neatly rather than piling it up. Research suggests this specialized signaling helps transform a rough, hasty repair into a seamless restoration.
Stopping the 'Infinite Alarm': How KPV Ends Chronic Inflammation Before It Causes Damage
Imagine a fire alarm that keeps ringing loudly long after the smoke has cleared. This is essentially what happens during chronic inflammation; your body gets stuck in "emergency mode," preventing the actual repair work from beginning. While some swelling is necessary to clean out bacteria immediately after an injury, the process must stop for true healing to occur.
The problem usually lies with tiny chemical messengers called cytokines. These proteins scream for attention to keep the immune system aggressive, but too many of them can damage healthy tissue. This is where the specific KPV peptide mechanism of action becomes vital. Acting like a site manager, KPV steps in to lower the volume on these loud messengers, effectively telling the immune cells that the crisis is over.
By silencing this false alarm, the anti-inflammatory benefits of KPV for skin repair unlock the next stage of recovery. The body can finally shift focus from fighting a nonexistent enemy to laying down fresh, healthy tissue.
The Software Update for Your Cells: How KPV Tripeptide Reorganizes Collagen for Smooth Repair
Once the "fire alarm" of inflammation is silenced, your body’s hardware needs specific instructions on how to rebuild the damaged area. The skin’s structure relies on the lysine-proline-valine effect on collagen remodeling to switch from emergency patching to architectural restoration. Think of KPV as a software update that uploads the correct blueprints to your cells, preventing them from rushing the job and leaving behind messy evidence.
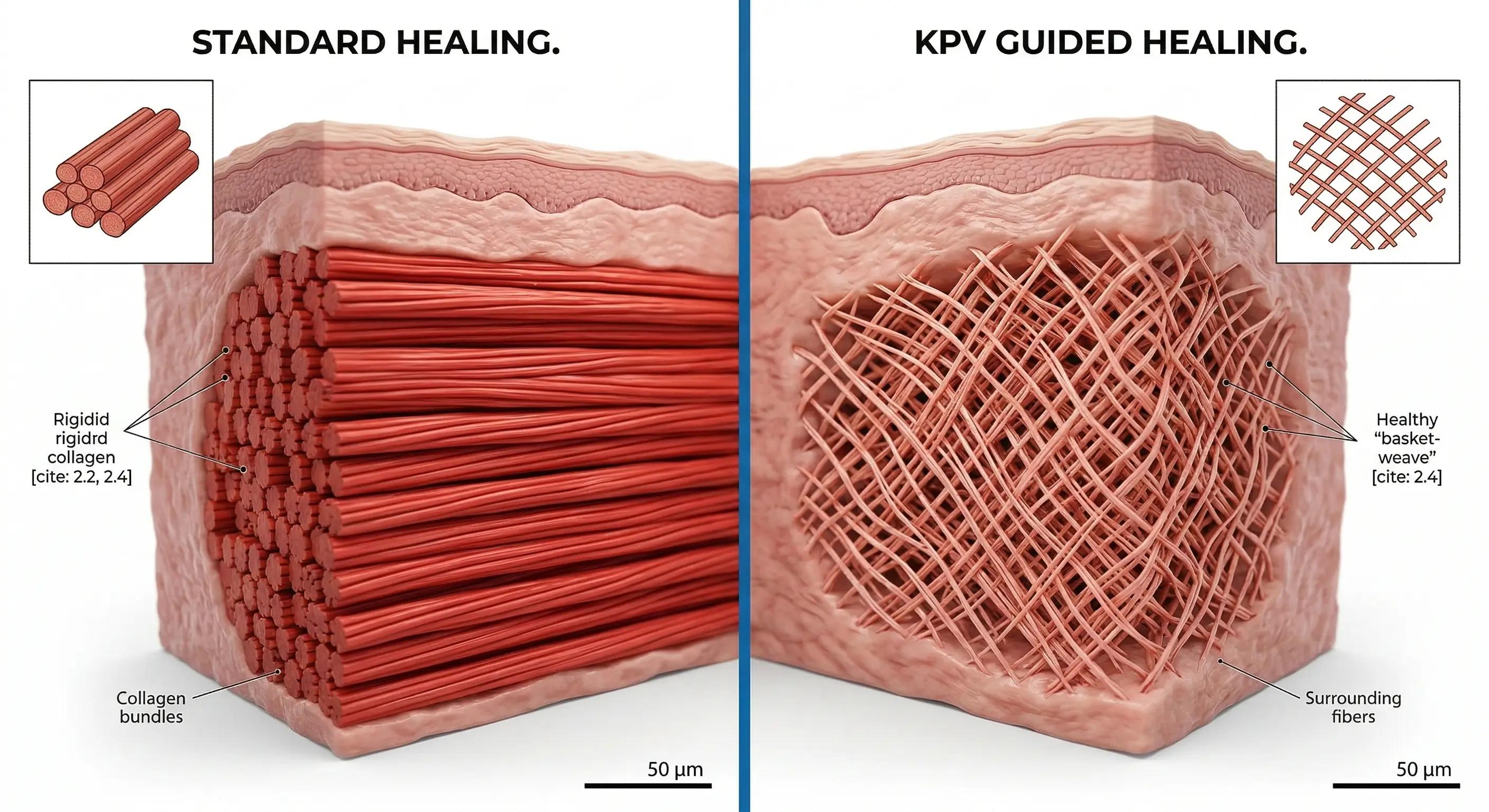
Construction duties fall to cells known as fibroblasts, which produce the "scaffolding" of your skin—technically called the extracellular matrix. Without proper direction, these cells tend to dump collagen in thick, parallel bundles that result in rigid, visible marks. The KPV tripeptide signaling for dermal fibroblasts changes this behavior, instructing these cellular workers to organize the material efficiently rather than just piling it up.
The role of KPV in extracellular matrix restoration creates a visible difference in the final quality of the healed skin:
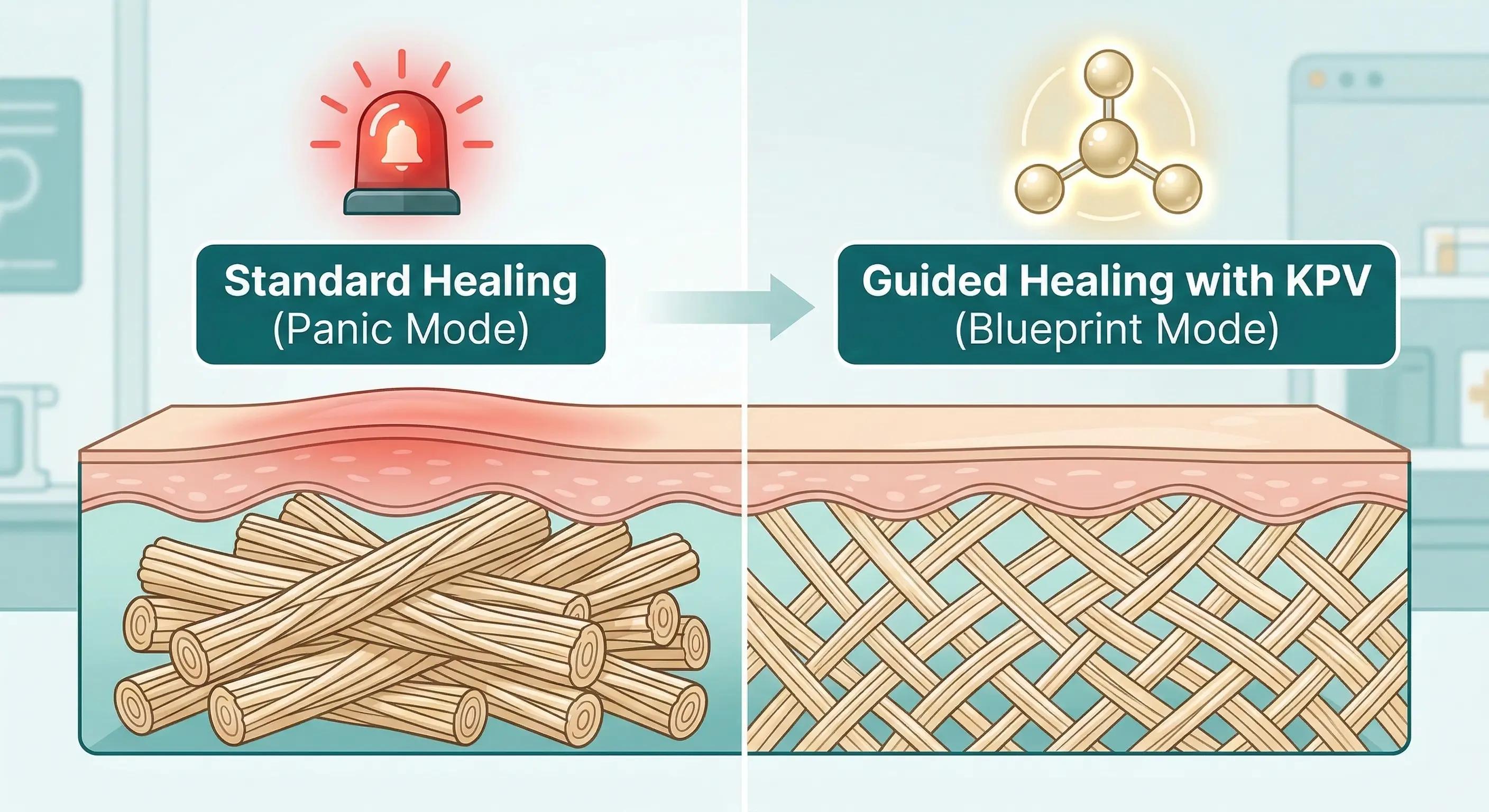
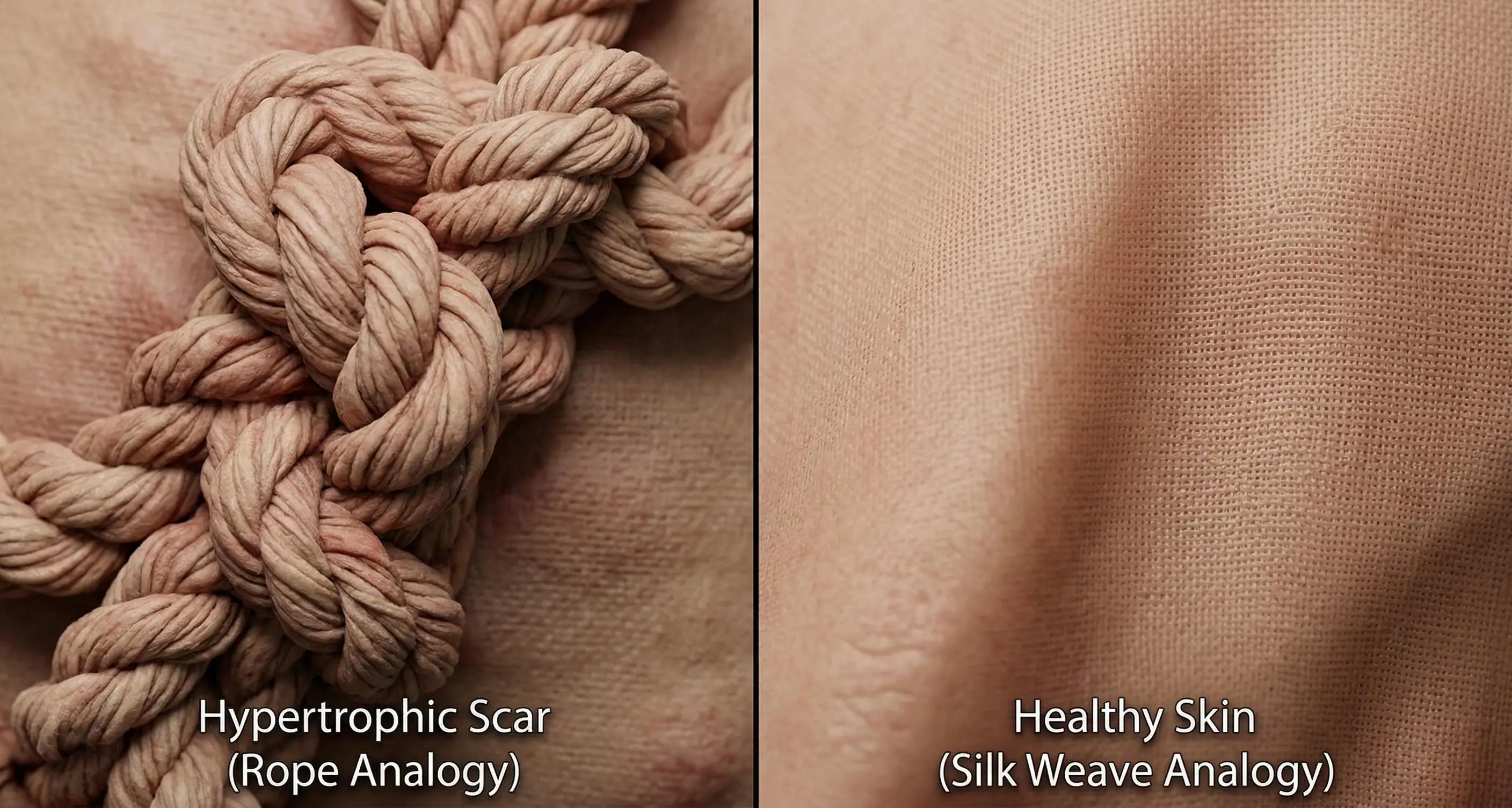
- Panic Mode (Standard Healing): Fibers stack like logs in a single direction, creating a raised, stiff texture.
- Guided Mode (With KPV): Fibers interlace like a wicker basket ("basket-weave"), allowing for natural stretch.
- The Outcome: Skin that regains its elasticity and blends seamlessly with the surrounding tissue.
From Lumpy to Level: Using KPV to Prevent Hypertrophic Scars and Keloids After Surgery
Most people assume unsightly marks result from the body not healing enough, but the thickest scars often come from the body doing too much. When your repair crew stays on high alert, they keep dumping building materials even after the gap is sealed, creating the raised, angry-looking mounds known as hypertrophic scars. Reducing hypertrophic scar formation with KPV works because the peptide acts like a rigorous project manager, cutting off the "pour more concrete" signal before the tissue piles up. This intervention is crucial for minimizing keloid risk after skin injury, as it prevents the excessive collagen buildup that turns a neat incision into a ropey, permanent reminder of your surgery.
While standard treatments like silicone sheets act merely as passive barriers to trap moisture, they fail to change how the underlying cells behave. Learning how to use KPV for surgical scar recovery offers a distinct advantage because it delivers an active biological command to stop inflammation at the source. Applying this signal once the wound has physically closed—usually a week or two post-operation—helps ensure the final repair remains flat and smooth rather than becoming a hardened overgrowth. This ability to regulate cellular activity is even more critical when the body’s healing process stalls completely.
Closing the Gap: Why KPV Is a Game-Changer for Stubborn Diabetic Ulcers and Non-Healing Wounds
While scars result from a system running overtime, diabetic ulcers represent the opposite problem: a repair crew that has gone silent. High blood sugar acts like static on a phone line, garbling the body's distress signals so that small cuts remain open for months. KPV tripeptide for chronic diabetic ulcers steps in to clear this interference, effectively "rebooting" the local cells to remind them they need to close the breach rather than ignoring the damage.
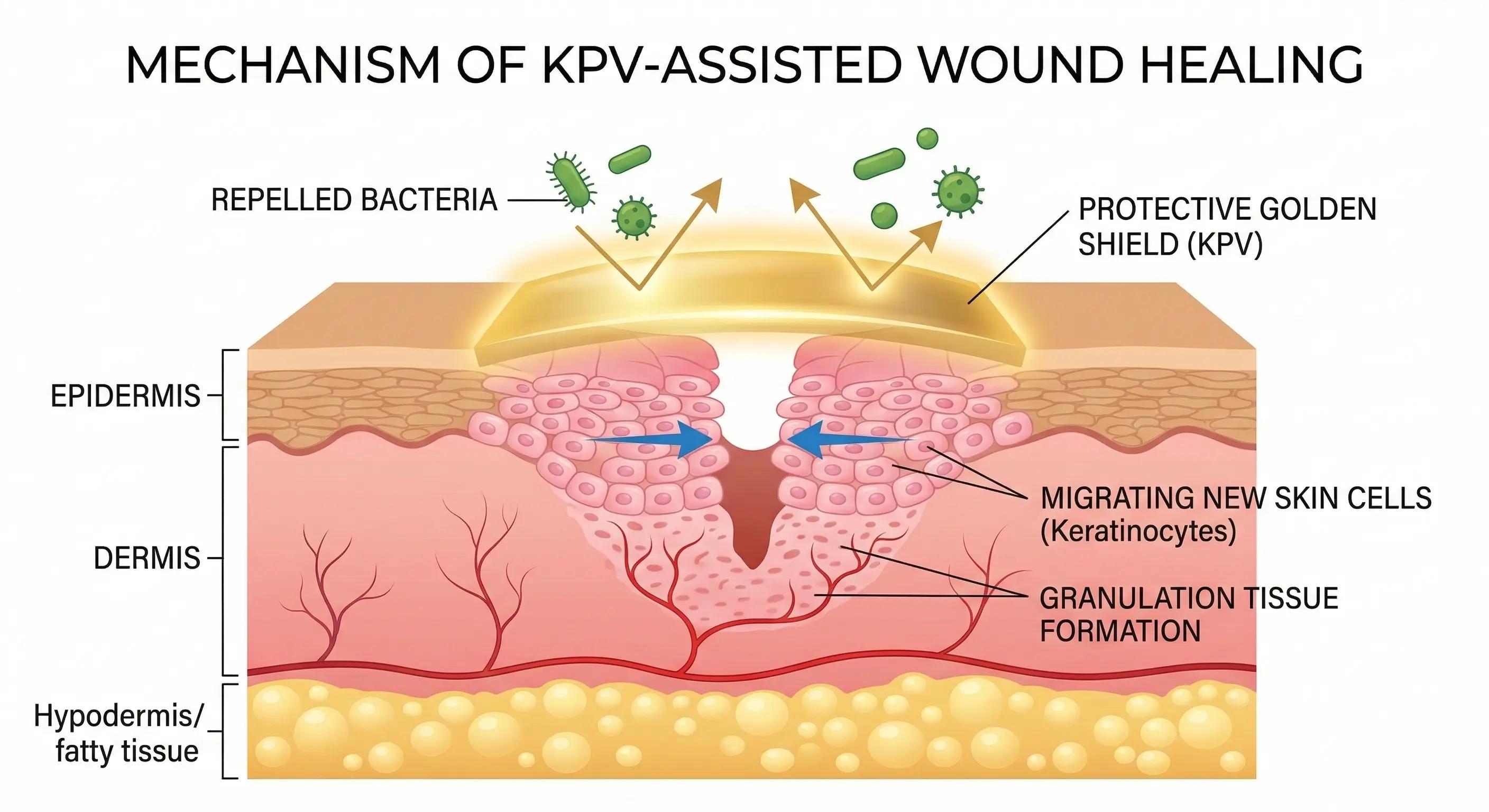
Managing non-healing wounds with antimicrobial peptides is particularly effective here because diabetic wounds are highly vulnerable to infection, which further halts recovery. KPV performs double duty by acting as a biological shield against bacteria while simultaneously instructing cells to resume construction. It specifically helps overcome these four common barriers:
- Reducing dangerous bacterial colonies on the wound surface
- Breaking the cycle of chronic, destructive inflammation
- Stimulating the migration of skin cells across the open gap
- Protecting the structural integrity of new tissue
This versatility places alpha-melanocyte stimulating hormone derivatives in dermatology at the forefront of treating complex skin issues. By functioning as both a defender against pathogens and a foreman for reconstruction, KPV offers hope for wounds that refuse to close on their own. Yet, for general systemic recovery, another peptide often enters the conversation.
KPV vs. BPC-157: Choosing the Right Peptide for Your Skin’s Specific Recovery Needs
BPC-157 often steals the spotlight as a "body protection" compound, but it functions differently than KPV. Think of BPC-157 as a logistics manager that excels at fixing internal infrastructure, like improving blood flow to damaged tendons or the gut. In contrast, comparing KPV and BPC-157 for tissue repair reveals that KPV acts more like a specialized architect. While BPC-157 handles the supply lines deep underneath, KPV focuses specifically on the surface, calming inflammation to ensure the final result looks smooth and organized rather than scarred.

For patients dealing with visible injuries, these two molecules can effectively work in tandem. Topical KPV applications for accelerated skin grafting are gaining attention because they manage the visible healing process directly at the source, distinct from systemic treatments. While the debate regarding KPV peptide vs traditional wound care treatments often highlights speed, the true advantage is precision: BPC-157 rushes nutrients to the site, while KPV ensures those nutrients build flexible, healthy skin ready for the next phase of your recovery journey.
Your 3-Step Roadmap to Faster Recovery and Healthier Skin with KPV
Treating KPV as a "software update" for your skin’s hardware transforms how you approach recovery. Instead of passively hoping a scar fades, you can now actively guide the repair process. By choosing this tripeptide over standard ointments, you address the root cause of scarring—uncontrolled inflammation—rather than just protecting the surface. Use this checklist to manage your next injury:
- Time it Right: Apply KPV once the wound closes to help the "site manager" organize collagen.
- Watch the Redness: Look for fading color and reduced heat as proof the inflammation alarm is quieting.
- Stay Consistent: Continue application through the remodeling phase to keep new tissue smooth.
Recovery is no longer a game of chance. By integrating this skin recovery plan, you leverage the precision of modern biotechnology to help your body heal not just faster, but better.